December 30, 2019
The National Center for Biotechnology Information defines high-value care as “the best care for the patient, with the optimal result for the circumstances, delivered at the right price.”1 Over the past few years, the expectation for high-value care has become formalized in national policies and regulatory mandates, yet it is still not the predominant standard of care.
Engaging healthcare providers in high-value care in 2020 will be critical for the U.S. healthcare industry.
Future reimbursement is at risk. The Centers for Medicare and Medicaid Services (CMS) and other payers have shifted toward value-based reimbursements. They use quality, cost, and efficiency measures to determine reimbursement. CMS has tied 5 percent of clinicians’ revenue in 2020 to their 2018 performance. The amount at risk will increase to 9 percent in 2022 based on 2020 performance.2
Healthcare costs are increasing. Global healthcare spending is projected to increase to $10.1 trillion by 2022. Estimates suggest $3 trillion of that money is spent on waste, for which the United States accounts for a third.3-4 Waste is any service, product, or process that does not help patients and is therefore unnecessary.5 Eliminating waste reduces cost and increases the value of care.
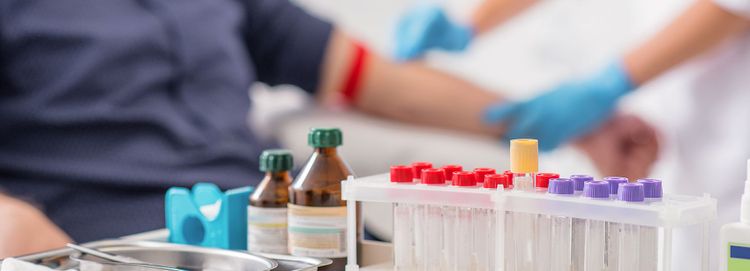
Overtesting and non-optimized prescribing cause patient harm. More than 770,000 injuries and deaths are caused by adverse medication events each year, costing as much as $5.6 billion.6 Making sure the right patient gets the right test or the right prescription at the right time is at the core of value-based care.
Successfully engaging healthcare providers in high-value care requires equipping them with knowledge and tools. We can start with education to guide providers toward ways they can participate in high-value care. The Choosing Wisely Campaign is a good resource for evidence-based recommendations.
Then we can put processes and checkpoints in place that reduce and eliminate waste while protecting patients from harm. Electronic health record systems can be valuable tools to automate high-value practices.
Finally, we can improve the accessibility and presentation of information used in clinical decision-making. Historically health system data has been anything but accessible. For years, data has been collected and defined by siloed entities in non-standardized and legacy IT systems. Health informatics, however, is increasingly connecting systems and allowing real-time analysis of this complex information.
hc1 is transforming lab data into personalized healthcare insights. The hc1 High-Value Care Platform™ eliminates waste and personalizes care for health systems and diagnostic laboratories nationwide by turning previously static lab data into actionable healthcare insights. Using the hc1 platform, health systems can improve clinical outcomes and reduce medical spend. Visit hc1.com to read more about the hc1 Platform and other high-value care initiatives.
References
- Committee on the Learning Health Care System in America; Institute of Medicine; Smith M, Saunders R, Stuckhardt L, et al., editors. (2013 May 10). Best Care at Lower Cost: The Path to Continuously Learning Health Care in America. Washington (DC): National Academies Press (US); 8, Achieving and Rewarding High-Value Care. https://www.ncbi.nlm.nih.gov/books/NBK207237/?utm_medium=referral&utm_source=r360
- Farah, MD, MHA, M. (9 Apr 2019). In search of high-value care: Six steps that can help your team. The Hospitalist. https://www.the-hospitalist.org/hospitalist/article/198542/leadership-training/search-high-value-care
- Leung, T. I., Merode, G.G. (2018 Dec 22). Value-Based Health Care Supported by Data Science. Fundamentals of Clinical Data Science pp 193-212. https://link.springer.com/chapter/10.1007/978-3-319-99713-1_14.
- Kimpen, J. (12 Feb 2019). Here’s how to make ‘value-based healthcare’ a reality. World Economic Forum. https://www.weforum.org/agenda/2019/02/here-s-how-to-make-value-based-healthcare-a-reality/
- Razmaria AA. High-Value Care. JAMA. 2015;314(22):2462. doi: https://doi.org/10.1001/jama.2015.16990
- World Health Organization. Patient Safety. https://www.who.int/news-room/fact-sheets/detail/patient-safety