09/15/20
Diversity in drug clinical trials and other drug research is important because patients often respond to the same dosages of the same drug in different ways. The drug can work exactly as intended in one patient with minimal side effects. Another patient might not see any improvement or, worse yet, might experience severe side effects. Documented variations in drug response help prescribers to determine which drugs will work best for their patients.
These variations occur because patients’ bodies process drugs differently. The term for this process is pharmacokinetics. Pharmacokinetics involves several stages: absorption, distribution, metabolism, and excretion. Patient characteristics and drug chemistry determine how pharmacokinetics work when a patient takes a prescription. For example, patients who metabolize a drug quickly may need a larger dose for the drug to work as intended or may need to take a different drug to see any benefit. Patients who metabolize the drug at a medium rate are likely to experience the full benefit of the drug. Patients who are slow metabolizers may need a smaller dose of the drug to avoid side effects or may not be able to take the drug at all because of the severity of side effects.
To help prescribers predict how a given drug will affect an individual patient, research has identified many patient characteristics that affect the pharmacokinetics of drugs. Age, weight, sex, liver and kidney function, and diet all have proven pharmacokinetic implications. Even with this information, prescribers face obstacles in determining the right prescription because many patient factors that affect pharmacokinetics are harder to pinpoint. As a result, patients often endure a prolonged trial-and-error prescription process as prescribers go through the cycle of adjusting dosages, monitoring effects, and trying different drugs until they find the right one to meet an individual’s needs.
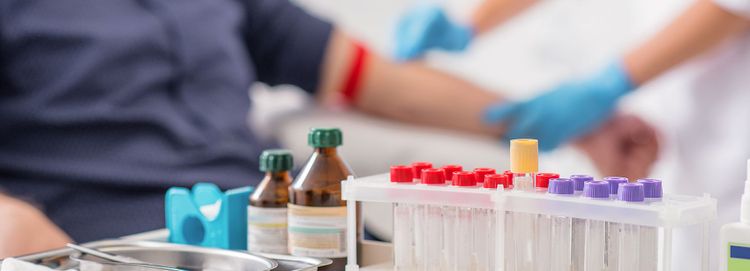
The goal of pharmacogenetics, which is the study of how variations in genes affect how a patient metabolizes certain drugs, is to prevent side effects and shorten the time it takes to establish the most effective medication plan for a patient. A pharmacogenetic (PGx) test involves taking a sample of the patient’s DNA and evaluating it for the genetic variations in the enzymes that metabolize drugs. The results of this test must be evaluated against current knowledge about how specific drugs interact with specific genes.
Developing this type of personalized medication plan across a large patient population takes coordination, organization, engagement, and monitoring, and that’s how the award-winning hc1 PGx Advisor® can help. It unifies PGx test results with the latest PGx drug information and facilitates patient engagement and monitoring to ensure that patients get the maximum personalized prescription benefit from PGx testing. Click here to learn more about how hc1 PGx Advisor® can improve patient outcomes while reducing overall medical costs.